When it comes to the health of our country, Chicken Little was right…the sky IS falling!
Read More"We Are What We Do" by Tim Church, M.D., M.P.H., Ph.D.
Living well and living long are two different things. and one of the country's leading preventive health researchers, Dr. Tim Church, states it plain and simple—maintaining a high quality of life means finding time for physical activity.
Dr. Tim Church, Holmes Murphy & Associates / ACAP Health Medical Director on exercising your right to a better quality of life
One of the things I've really learned in medicine is that there are certain things that resonate with us that we believe in, with or without data – it just must be true. And the idea of, 'we are what we eat,' it is amazing to me how people hold onto that. People have a hard time getting their arms around, 'we are what we do.'
As a physician, through med school, through residency, I just got frustrated with treating things that were 100 percent preventable. And, you know, I love to say we like to heroically clean up after the car accident, but we don't like to put up stop signs. And, I just was always drawn towards prevention and then in my prevention quest so to speak, physical activity and exercise just made so much sense. It didn't matter what the analysis was. It didn't matter what we were looking at. There was always this one variable that was so powerful. It was exercise.
When it comes to weight loss one of my favorite sayings is: you diet to lose weight, and you exercise to keep it off. It doesn't matter what the macronutrient components of that diet are. You can focus on low carbs. You can focus on low protein. You can focus on low fat. It doesn't really matter. It tends to be an individual thing.
But, once you get the weight off, exercise becomes so critical in keeping it off. It's not hard to lose weight. It's very easy to lose weight, that's why all the fad diets work. That's why all this bogus stuff works. The challenge is keeping the weight off, keeping it off at six months, keeping it off at 12 months, keeping it off at two years.
Everything counts. If you're doing nothing now, this is not all or nothing, this is not about, 'hey if you don't get to 150 minutes a week, then it's a waste of time.' Just getting off the couch has benefits. In fact, the most sedentary individuals who have the worst health are the ones that benefit the most from a little bit of physical activity. The return on investment for a little bit of physical activity is huge for those guys. The person who's running a 10K all the time and ramps it up to a marathon. They don't get any more benefit when they go from 10K to marathon, they've already kind of maxed out. But that person who's totally sedentary and takes up a walking program? Huge benefits.
It's not about how long you're gonna live. How long you're gonna live is primarily determined by how long your grandparents lived, how long your parents lived. It's about how long you live well. Can you go duck hunting in your 80s? Can you chase your grandkids? You know, can you do the things that you love doing? And there's no pill for that. We can't go to the doctor and get a pill for quality of life. There's one thing we know that works for maintaining quality of life. And that is being physically active. That is leading an active lifestyle which may or may not include formal exercise. So, you want to lead the life you want to lead? You've got to be physically active.
© 2014 ShareWIK Media Group, LLC. All Rights Reserved.
Benefits Insight from a Twitter Founder
 Jack Dorsey, the founder of Twitter (and now Square) once famously quipped that as business leaders we should "make every detail perfect and limit the number of details to perfect".
As employee benefit advisers, human resource and benefit professionals and service providers deal with new regulations, burden shifting and changing roles in a fast-changing employee benefits industry, we sometimes lose sight of who we are serving. As long as an employer is paying the majority of the costs, the employee benefit programs is an investment that reflects the culture and value placed upon the people in the organization.
Jack Dorsey, the founder of Twitter (and now Square) once famously quipped that as business leaders we should "make every detail perfect and limit the number of details to perfect".
As employee benefit advisers, human resource and benefit professionals and service providers deal with new regulations, burden shifting and changing roles in a fast-changing employee benefits industry, we sometimes lose sight of who we are serving. As long as an employer is paying the majority of the costs, the employee benefit programs is an investment that reflects the culture and value placed upon the people in the organization.
It might surprise some business owners to learn that the "perceived" value of the benefits actually has less to do with the family out-of-pocket amount and office visit copay and more to do with benefit experiences throughout the year. This was reinforced through a study by Deloitte that identified the high direct and indirect expense of turnover when good people leave their jobs because of bad management and poor culture. Employee benefits did not even make the top ten list of the reasons to jump ship.
Sure, getting the benefits design of your programs to reflect your company's core beliefs is an important first step along with selecting the right service providers and making sure we are in federal and state compliance. But all too often we run out of time to pay attention to the details that matter most ... the enrollment and user experience for our customer. Selecting a plan provider and paying the majority of the premium is hardly where the responsibility ends.
Have you seen this before in your benefit materials ... Call this number to set up an appointment, fax this form to this group, set up another user name and password to qualify for this, watch this video and fill out this form to get this, do these 10 meaningless things that will not impact your health ... and my favorite ... read this ... but don't take any action now (I just want you to inform you of these things that will add more stress to your world ... along with work and family obligations, missing planes, Ebola viruses, impending Cold War and Middle East unrest) but check back later for more details from your HR team. Also, plan to keep an an eye out in your inbox for more important dribble about your employee benefits that does not have any call to action or benefit to you or your family members.
Jack Dorsey gets it right ... because he cares about the ultimate detail, design and user experience. Twitter was about a simpler way to communicate. Square and Apple Pay are trying to improve the buying experience. When it comes to delivering employee benefits, we are always on target if we ask how we can make the service experience better for those whom we serve.
No Health Insurance - IRS Shows Us How Penalty Is Calculated
 If your like me ... you may have thought the IRS penalties imposed for not having health insurance under the new ACA federal healthcare rules simply utilized the greater of 1% or $95 calculation by applying 1% times adjusted gross income.
If your like me ... you may have thought the IRS penalties imposed for not having health insurance under the new ACA federal healthcare rules simply utilized the greater of 1% or $95 calculation by applying 1% times adjusted gross income.
This week, Ed Oleksiak, JD, Holmes Murphy's national compliance lead, walked our consulting teams through how the the IRS will apply the penalty. So the 1% individual penalty is not just 1% times your income. You actually subtract a base amount which is the minimum thresholds for being required to file a tax return determined by filing status and then the 1% is multiplied times the resulting net income amount. The starting amount is household income. We are including a definition and example below.
Household income is the adjusted gross income from your tax return plus any excludible foreign earned income and tax-exempt interest you receive during the taxable year. Household income also includes the incomes of all of your dependents who are required to file tax returns.
Example: Single individual with $40,000 income
Jim just plain does not like politics or federal mandates. He is an unmarried gun-toting, iPhone 5s carrying young invincible with no dependents. He pays service fees each month to access his Match.com account ... but feels paying monthly health insurance premiums does not help him with the ladies. Jim does not have minimum essential coverage for any month during 2014 and does not qualify for an exemption. For 2014, Jim's household income is $40,000 and his filing threshold is $10,150.
To determine his payment using the income formula, subtract $10,150 (filing threshold) from $40,000 (2014 household income). The result is $29,850. One percent of $29,850 equals $298.50.
Jim's flat dollar amount is $95.
Because $298.50 is greater than $95 (and is less than the national average premium for bronze level coverage for 2014), Jim's shared responsibility payment for 2014 is $298.50, or $24.87 for each month he is uninsured (1/12 of $298.50 equals $24.87).
Jim will make his shared responsibility payment for the months he was uninsured when he files his 2014 income tax return, which is due in April 2015.
2014 Federal Tax Filing Requirement Thresholds
|
Filing Status |
Age |
Must File a Return If Gross Income Exceeds |
|
Single |
Under 65 |
$10,150 |
|
65 or older |
$11,700 |
|
|
Head of Household |
Under 65 |
$13,050 |
|
65 or older |
$14,600 |
|
|
Married Filing Jointly |
Under 65 (both spouses) |
$20,300 |
|
65 or older (one spouse) |
$21,500 |
|
|
65 or older (both spouses) |
$22,700 |
|
|
Married Filing Separately |
Any age |
$3,950 |
|
Qualifying Widow(er) with Dependent Children |
Under 65 |
$16,350 |
|
65 or older |
$17,550 |
Health Plan Identifier (HPID) - A Must Do by November 5th, 2014
If your company sponsors a health plan (excluding small plans), and you have administrative oversight of that plan, you must get a Health Plan Identifier (HPID) under HIPAA by November 5th, 2014. You might be saying, I already have a lot on my plate or I would rather wait to do this in November. Sure, you could wait until things get slower around the fall during open enrollment or look into this before the holidays. Or you or a member of your HR/Benefits team could knock it out today.
Here are the instructions our firm put together to assist our clients.
This is being required by our federal government ... don't shoot the messenger ... we are simply trying to urge our clients to do this now.
Carrots and Sticks are for Donkeys and Mules
The following is a must watch for anyone who endeavors to change the health risk of a population. Our industry needs to move beyond treating our people like they are asses. We assume humans are like farm animals motivated by dangling a carrot or giving a smack on the rear. As Dr. BJ Fogg explains in the video below, an employee's level of motivation is hardly the culprit.
The research and understanding of "B=MAT" - behavior = motivation, ability and trigger ... is worth the small time investment it will take to watch this video. Dr. Fogg’s research is some of the most groundbreaking in terms of how human beings change behavior. Dr. B.J. Fogg is the Director of the Persuasive Technology Lab at Stanford University.
I came across this video at Rock Health when launching my own startup in the digital health technology space.
The HSA Turns Ten
 There are some larger than life personas residing in Dallas who have had a profound impact on shaping our nation's health care system. It was December of 2003 when President Bush had just signed into law the Medicare Prescription Drug Improvement and Modernization Act. John Goodman, head of the Dallas based National Center for Policy Analysis (NCPA), helped give birth to provisions of the bill having contributed much of the thinking around HSA's and how a consumer's right to vote with their own pocketbook could change the health care marketplace.
While Goodman may have been the mother who conceived of the HSA and George W. Bush the father of the bill, this tax-advantaged baby got delivered to my team's front door step while consulting with a Fortune 500 client out of Austin, TX. It was 2003 and this company's leadership team was wrestling with an unsustainable health trend and a culture ready for change. They were the first and largest company in Texas to launch a qualified High Deductible Health Plan (HDHP) with an HSA in 2004. From conception of the design to the final delivery to employees, this work was significant and groundbreaking as employees at this company began to learn to use insurance for its intended purpose.
There are some larger than life personas residing in Dallas who have had a profound impact on shaping our nation's health care system. It was December of 2003 when President Bush had just signed into law the Medicare Prescription Drug Improvement and Modernization Act. John Goodman, head of the Dallas based National Center for Policy Analysis (NCPA), helped give birth to provisions of the bill having contributed much of the thinking around HSA's and how a consumer's right to vote with their own pocketbook could change the health care marketplace.
While Goodman may have been the mother who conceived of the HSA and George W. Bush the father of the bill, this tax-advantaged baby got delivered to my team's front door step while consulting with a Fortune 500 client out of Austin, TX. It was 2003 and this company's leadership team was wrestling with an unsustainable health trend and a culture ready for change. They were the first and largest company in Texas to launch a qualified High Deductible Health Plan (HDHP) with an HSA in 2004. From conception of the design to the final delivery to employees, this work was significant and groundbreaking as employees at this company began to learn to use insurance for its intended purpose.
According to the Employee Benefits Research Institute (EBRI), since the bill was signing into law, HSAs have since grown to 16.6 billion dollars in assets. In 2013, these assets grew 5.3 billion, a jaw dropping 47% increase over 2012 assets. Meanwhile, Health Reimbursement Arrangements (HRAs) are moving in the opposite direction with assets shrinking by 2% to 5.7 billion dollars last year.
There is a massive shift taking place in the market as consumer's continue to shoulder more of the out-of-pocket expense of health care and demand greater transparency over quality and cost. It has forced hospitals and physicians to cope with collections and bad debt since "we the people" are not always as reliable paying our bills as a large insurer. HSA linked plans have also sparked innovations from new swipe-card technology to alternative forms of free market care delivery.
While our country's legislators and many employers are currently fixated on purchasing health insurance, the real challenge over the next decade will be how incentives can be aligned to produce systemic behavior change that leads to the reduction and production of disease.
In 2013, more than 15 million individuals were enrolled in HSA-linked plans, a 50% increase in just three years. In 2014, reports indicate about 18% of employees will enroll in a tax-advantaged accounts linked to a high deductible plan. Here are a few reasons why HSA's will continue to thrive over the next decade:
1. Taxes are high - Marginal tax rates are at 39.6% and corporate taxes exceed those of other industrialized countries. Adopting tax-efficient plan design strategies like maximizing annual and catch-up contribution limits and using captives where appropriate will make sense for astute plan sponsors who care enough to reduce their own corporate and their employee's tax burden.
2. Qualified High Deductible Plans Are No Longer "High" - The minimum deductible and out-of-pocket requirements may have seemed high in 2003, but the 2014 minimum annual deductible of $1,250 is not that far from the $1,100 average annual deductible nationwide and well below the $1,700 average for small firms (under 200 workers). By the way, just because the legislators called it a "high" deductible health plan does not mean you need to promote it as such when you roll it out to your employees. Ask your benefits communication team to come up with something snappier.
3. They cost employers less - HSA linked plans cost employers about $1,700 less per employee compared with traditional PPO plans, according to a 2013 Mercer survey. In one of the first studies of its kind, EBRI found HSA linked plans reduced total health care spending by 25% in its first year and over the succeeding three years — albeit at a slower pace.
So Happy Birthday HSA ... It's time to toast you and those who nurtured you to ten. Here's to another a decade of market-driven progress enabling those who take measurable steps to improve their health to continue investing in themselves.
Health Care Pricing ... All Over the Map
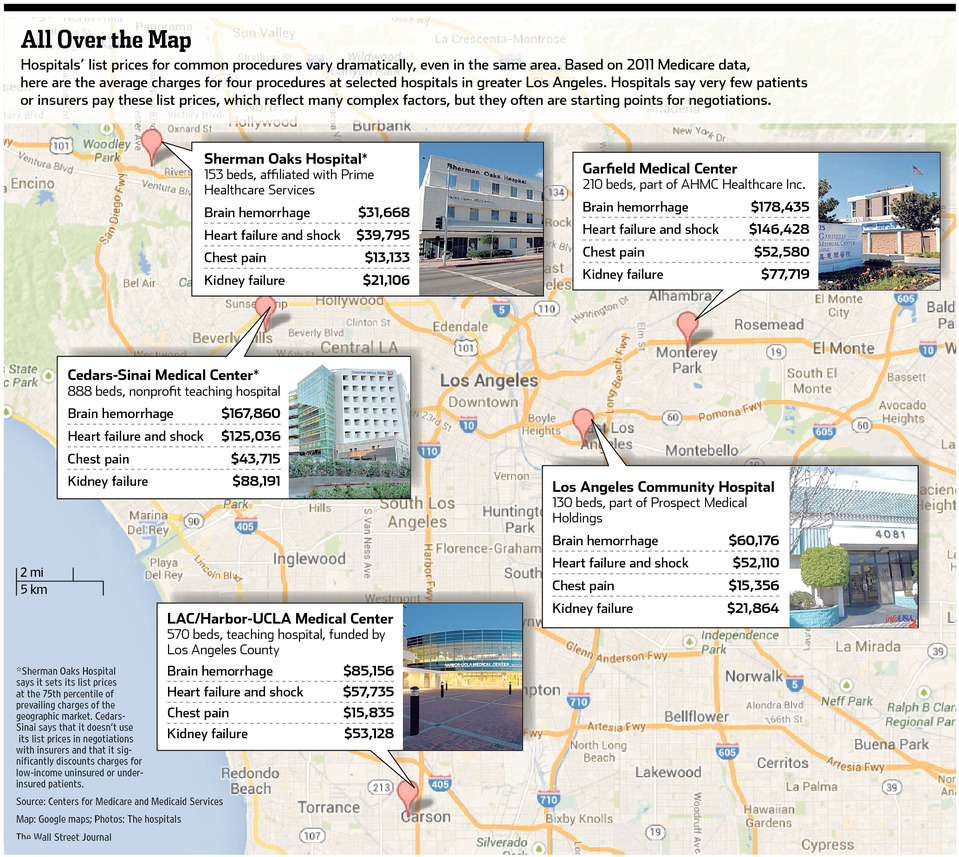 It's always fun to watch shoppers each holiday season camp out for hours to snap up bargains that pale in comparison to the savings available in the health care marketplace. If buyers put as much emphasis on shopping for health services throughout the year as we do on enrolling for coverage once a year, we could make greater strides to flatten the cost trajectory of care.
If there is one city that knows how to shop it's Big D, so here's a three-step process for any employer hoping to put a little "Black Friday" in their health plan:
It's always fun to watch shoppers each holiday season camp out for hours to snap up bargains that pale in comparison to the savings available in the health care marketplace. If buyers put as much emphasis on shopping for health services throughout the year as we do on enrolling for coverage once a year, we could make greater strides to flatten the cost trajectory of care.
If there is one city that knows how to shop it's Big D, so here's a three-step process for any employer hoping to put a little "Black Friday" in their health plan:
1. Offer A High-Deductible Plan:
A 'quiet revolution in health insurance' is taking place as the number of employees enrolled in a plan with an annual deductible of $1,000 or more has risen to nearly 40% in 2013. Among all plans, the average annual deductible among covered workers is over $1,100 and exceeds $1,700 for small firms (under 200 workers). (Kaiser/HRET Survey of Employer Sponsored Health Plans).
Milton Friedman wisely quipped "Nobody spends somebody else's money as wisely as he spends his own. Putting in a high deductible plan enables your employees to be economically rewarded for shopping around and strategically aligns your insurance plan to cover infrequent and high cost medical events.
2. Arbitrage your Network
In the 20th century days of health care consulting, we used to attend to great detail to reprice claims for employers wanting to select the right insurer and network health plan. This focus on network discount has given way to more sophisticated value equation models. Once your health plan/network is in place, the employer must then teach employees to exploit hidden value within the network throughout the year.
60% of medical and pharmacy claims come from non-emergent services. As an example, three facilities within a five-mile radius in Dallas offer the same in-network MRI for prices ranging from $600 to $3,000. Transparency laws are now enabling big data analytics software to quickly review over a billion national claim records for price and quality comparisons at the push of a button.
3. Shop with a trusted friend
The best health price transparency providers have realized that shopping for care is best delivered when technology is married with an independent consumer advocate. As an example, there are over thirty types of knee surgery, so having a personal concierge to help me navigate my options enables my family to build trust with an advisor that does not have a financial interest in the outcome. To revolutionize the system, we need to help our employees act on information, not just provide data.
Many DFW employers are well on their way to creating a shoppers mentality among their health plan enrollees. Consumer advocacy and pricing transparency programs have already returned annualized savings anywhere from four to twenty-four times the cost of the service.
In a town that continues to reinvent the shopping experience, we anticipate more companies to get on the "Black Friday" bandwagon when it comes to savings in their health plan. The best part is we can all be empowered to score health deals that would make a Walmart clerk gush just by picking up the phone.
Top Ten Healthcare Predictions for 2014
 1. With UT falling to Baylor, another 50/50 season for the Dallas Cowboys and a botched HealthCare.gov rollout in 2013, predictions for 2014 have head coach, Jason Garrett and U.S. Secretary of Health and Human Services, Kathleen Sebelius joining the ranks of Mack Brown and the unemployed ... At least they will have a new health insurance option available to them when they leave their employer.
2. Consumer health devices, mobile and telehealth initiatives will continue to bring about market-based reforms that enable better tracking, monitoring, and care coordination for patients with chronic conditions, who lack access to primary and specialty care or for those payers and providers willing to experiment with technology enabling solutions.
1. With UT falling to Baylor, another 50/50 season for the Dallas Cowboys and a botched HealthCare.gov rollout in 2013, predictions for 2014 have head coach, Jason Garrett and U.S. Secretary of Health and Human Services, Kathleen Sebelius joining the ranks of Mack Brown and the unemployed ... At least they will have a new health insurance option available to them when they leave their employer.
2. Consumer health devices, mobile and telehealth initiatives will continue to bring about market-based reforms that enable better tracking, monitoring, and care coordination for patients with chronic conditions, who lack access to primary and specialty care or for those payers and providers willing to experiment with technology enabling solutions.
3. Watch for continued M&A activity with health systems similar to Baylor Scott & White or Tenet (Vanguard Health) in other areas of the country. Health care delivery systems will continue to survive and thrive through specialization, mergers, or partnerships that lead to even bigger systems of care.
4. After the elections in November 2014, more carriers will exit the exchange system or become even more selective with their markets and propose double digit premium rate increases as the demographic underpinnings of the exchange fail to capture the 18-34 age group needed for the law to succeed.
5. With less than predicted young people signing up for HealthCare.gov, watch for legislative push to increase penalties for those who did not adhere to the requirements in the law in 2014. There will also be a healthy amount of debate over whether the penalties should be waived in 2014 due to the botched website rollout of healthcare.gov. [The penalty for 2014 is the greater of $95 a year or 1% of adjusted gross income].
6. The political rhetoric of "repeal and replace" will eventually give way to the demands of the American people searching for bipartisan amendments and solutions that target the real enemy in this country ... a broken fee for service environment that pays for the reimbursement of treating disease. The government will not shut down in 2014.
7. Employers will continue to adopt tax-efficient plans (such as high deductible health plans with health savings accounts) as new taxes (associated with ACA's funding) become more transparent to higher wage earners. Private health exchanges will grab the attention of employers interested in defined contribution approaches to funding their benefits.
8. Companies will abandon large incentives associated with traditional first generation wellness offerings (HRA's, Biometrics, and Wellness Content) in favor of programs that actually show promise of changing behavior to combat the effects of smoking, obesity, metabolic syndrome and diabetes — Pharmacotherapy and surgical options will gain more traction for those who qualify.
9. Watch for the continued proliferation of programs that provide price transparency and consumer advocacy. Consumers and large payers will become more educated around the disparity in pricing among health care facilities and providers. Congress will try and respond with everything from price controls to transparency bills.
10. Congress will not be able to agree to the Medicare cuts that are the underpinnings of the Affordable Care Act. The Office of Management and Budget (OMB) will run new actuarial calculations that increase the size of the federal deficit beyond what our children can bear.
The One Thing Needed for Exchanges to Succeed
Young people are the most coveted of all participants to have enrolled in a health insurance plan. It is the concept that underlies group underwriting to have those with fewer health risks to help offset the cost of those who are older and have greater medical needs. Dallas ranks as one of the largest communities of uninsureds in Texas at 31% compared to a 26% state average. Many of these uninsureds are young people (ages 18-35) who have relied on our public health system to be there if things do not go as planned.
The very success of the Affordable Care Act (ACA) will depend upon convincing these "young invincibles" that health protection is worth purchasing. If only the public exchanges could be as inviting as an Abercrombie & Fitch, Hollister or a Juicy Couture. The federal government is projecting enrollment in the exchange system to be around 7-8 million by the end of 2014. As the law intends, the cost of insuring the most expensive users of the system must be offset by around 2.7 million of young invincibles between the ages of 18-35 for it to work. In the first month of enrollment, 26,794 people selected a health plan on the federal exchange website. The makeup of these enrollees has not been released by the federal government, but a demographic match to the patronage of a cafeteria restaurant is to be expected.
As exchange enrollment begins to materialize in 2014, public officials may wish to revisit the following if they hope to enroll the most coveted young adults:
1. A Retail Experience That Works - When the standard young people are used to is designing their own Nike shoes online or ordering Uber's transportation service at the push of a button, HealthCare.gov will find itself quickly falling off the browser's "favorites" list. In a November survey by USA Today, many young people will not try again until December and cannot even comprehend calling a 1-800 number for service. We all like using intuitive technology that works ... but young people demand it even more ... a problem plaguing HealthCare.gov for the foreseeable future.
2. Changes to Employer Plan Dependent Definition - Many employer plans used to only cover dependent children up to age 19 or 26 (if a full-time student). On January 1, 2014, all employers (grandfathered and non-grandfathered) will be required to extend coverage to dependents up to age 26. The chief actuary at CMS is likely regretting the legislature's decision to extend dependent coverage to age 26 for employers. With 60% of American's covered by employer-based plans, this leaves a smaller group of of younger adults to enroll under the public exchanges.
3. Affordable Coverage - Older Americans will pay a higher rate than younger Americans, but the community rating is tiered using only three different age group bands. AARP lobbied strongly for this and it is an absolute boon to the baby boomers and a real shaft to Generation X, Y, and millennials who will bear the brunt of the top third-oldest risk tier by age. Age rating bands of 3:1 will prevent insurers from charging an adult age 64 more than three times the premium they charge a 21-year-old for the same coverage. As a result, young Americans will see higher premiums under the Exchanges than when they could have purchased coverage (Pre-ACA) in the private market when they used age rating bands of 5 to 1.
The Obama administration's federal study found that if all 50 states had expanded their Medicaid coverage the way they were supposed to when the law was passed, almost 90 percent of single Americans under 35 years could get coverage that cost less than $100 a month. They did not count on a Supreme Court ruling that enabled 25 states to opt out of expanding Medicaid coverage. This created unexpected "cracks" in the system when many young people who were to have qualified for Medicaid coverage will find they do not earn enough for subsidies under the Exchange.
In an astute political move, the Obama administration pushed back the requirements to release projected increases in health premiums for 2015 until after the November 2014 elections. In 2014 our young adults will eventually have to make a decision to pay the federal penalty (the greater of greater of $95 or 1% of AGI annually) or buy health coverage. Here's betting their XBox One they pay for neither.
Struck by Turtle? There's a Code for That

GOVERNMENT UPDATE: LIKE MOST REFORMS CONTROLLED BY A HEAVY HANDED BUREAUCRACY ... RULES WERE CHANGED MIDSTREAM PROMPTING OUR FREE MARKET SYSTEM TO REACT AGAIN TO UNEXPECTED CHANGES IN THE WAY HEALTH CARE IS REGULATED. THIS WAS THE RIGHT CALL TO DELAY THIS GIVEN BURDENS PLACED ON OUR CARE GIVERS . - APRIL 2014
The U.S. health care system will be implementing a new coding system called ICD-10 that is scheduled to take effect on October 1, 2014. The Centers for Medicare and Medicaid Services (CMS) will require the code sets be used by any covered entity under HIPAA (Health Insurance Portability Accountability Act). Whenever we are treated for medical care, a code is assigned to designate our illness or injury. These diagnosis codes are meant to help providers and payers better track what happened, how much it should cost and what follow-up care is needed.
The ICD-10 codes will not impact coding for outpatient procedures and physician services. There are around 13,000 codes under the current ICD-9 code set and an additional 55,000 coming next year. While the new 68,000 codes will yield enhanced reporting, the real beneficiaries in 2014 will be the IT providers who will charge more to implement the new CMS standards in their EMR systems. These costs will get passed along to payers and consumers in the form of higher prices for treatment.
Since our U.S. government is providing plenty of comedic fodder, it seemed like a good time to pile on and share some of our favorite codes:
- Struck by turtle, initial encounter: W5921XA
- Struck by turtle, subsequent encounter: W5922XD
- Hurt at the opera: Y92253
- Stabbed while crocheting: Y93D1
- Walked into a lamppost: W2202XA
- Walked into a lamppost, subsequent encounter: W2202XD
- Submersion due to falling or jumping from crushed water skis: V9037X
One of my favorite groups of codes relates to the rampant incidence of space-related injuries we often hear about. Thank goodness there are over ten codes for when a spacecraft goes out of control and plays a role in an injury. If you collided your spacecraft the first time use V9543XA. Do it once more and the hospital staff needs to use V9543XD for a subsequent encounter. How about codes for injuries with Macaws, Centipedes ... and others animals with from fur to feathers ... are available here.
Over 40 medical specialty groups, state organizations and the American Medical Association (AMA) have written letters to CMS recommending they cancel the implementation of ICD-10. The concern is that the new codes will "create significant burdens on the practice of medicine with no direct benefit to individual patient care." Additionally, the letters cite the burden of code implementations on top of a growing list of challenges doctors and hospitals have with the 2014 implementations of federal and state health care reforms.
So the next time you're injured from the dangers that lurk within the Winspear Opera House or you suffer a "burn due to flaming water-skis" ... just know that your federal government has you covered.
Photo Courtesy of PBS Newshour
Consumer Reports - Health Exchange Guidance
It seems ironic that we are on the eve of the October 1st, 2013 launch of the largest public open enrollment of health insurance in U.S. history and we are one day away from a government shutdown. While the rest of Washington D.C. tries to get its act together, we recognize that our friends in human resources may need a trusted resource to help navigate consumers through the impact of the Affordable Care Act (ACA). This year only, the health exchange marketplace open enrollment period will run from October 1, 2013, through March 31, 2014. In subsequent years, open enrollment will run from October 15th through December 7th, for a January 1st effective date. After this initial year only, the October 15th open enrollment schedule will match up with that of Medicare.
The older I get the more I rely on unbiased experts who can save me time and have my best interests at heart. This is why I am a subscriber to Consumer Reports. In the November 2013 issue, I was pleased to find a well constructed explanation of the ACA and how it might impact three different groups: someone who gets insurance through work, who buys insurance on their own, or who is Medicare eligible.
With over twenty years of benefits consulting experience, I thought I would put the Consumer Report's online guide called healthlawhelper.org to the test. I am giving it an enthusiastic thumbs up and hope you share it with those who come to you for help. It is a free resource that offers an easy to follow questionnaire that guides consumers through a personal decision making process on what to do. Consumer Reports is a national nonprofit organization with one and only one mission: to take the side of consumers wherever they may need it. Since the new health law is the biggest change in the American health care system in more than a generation, they created the Health Law Helper to give consumers accurate and unbiased information about the law and how it affects them.
Please pass it along to anyone who needs advice from a trusted organization with the consumer's best interest at heart.
Health Exchange Marketing - Finding SuperMan or (Woman)?
October 1st, 2013 marks the official kick-off of the open enrollment window for eligible Americans to enroll for health insurance through state exchanges for a January 1, 2014, effective date. The hope of course is that 40 million uninsureds sign up or they will face a penalty of the greater of $95 or 1% of adjusted gross income. The odds makers are projecting somewhere between 7-8 million enrollees will hit the buy button for 2014. While federal navigators and the administration will be touting how to enroll ALL Americans, the insurance carriers who have selectively chosen their markets will take a different tactic. If history repeats itself, the last mass public-private health enrollment push dates back to the Bush-era when Medicare Advantage plans first became available to the over 65 crowd. A regulatory official once shared with me they had to take enforcement actions against an insurance company promoting their Medicare Advantage plans after learning the carrier held their informational meetings on the top floor of a strip mall with stair-only access. Ask yourself if you would rather insure a senior citizen that can walk up a flight of stairs or one that rolls onto an elevator in the latest personal electric transport chair endorsed by Burl Ives? This post is not meant to judge our for-profit businesses for pursuing legal tactics that enhance profitability for their shareholders. Profit or perish is the maxim for any business. The far greater concern is what happens when public and private insurance pools go after the best customers. History shows us that private enterprise usually wins out when it comes to marketing consumer goods and services.
The big five health carriers are poised to spend $1 billion or more to attract millions of new customers who never have payed health premiums before. Despite the appeal of a glossed-up "Kathleen Sebelius flyer" produced by the Secretary of Health and Human Services office for "Navigator" distribution, finding "Superman" will not be a fair gunfight for the public Exchanges. Let's face it ... the Madison Avenue-style advertising budgets funded by the largest insurance carriers will be playing in a different league. If you haven't noticed ... the largest health carriers are now sponsoring more marathons, cycling teams, triathlons, mob and ultra events than ever before. It's health marketing 101, the audience there is worth the brand impression.
Don't expect to see a carrier-sponsored exchange ad next time you're picking up your blood pressure meds at the local CVS. Instead, check inside a Men's Health or Seventeen magazine to find out how to enroll ... or better yet ... run a local 10k and post your results on your Facebook timeline. The chances are in this new digital economy, there is already enough "big data" that is aggregated on you to predict your health risk. You will know your health status by how aggressively you are sought after.
Is the obesity crisis hiding a bigger problem?
From Leonardo da Vinci to Dr. Atkins, society often ridicules those with different points of view. Here Dr. Peter Attia discusses some compelling reasons why we might want to question the conventional thinking around obesity and insulin resistance. Dr. Peter Attia's presentation has nearly garnered 1MM views and it's worth the watch.
As a young surgeon, Peter Attia felt contempt for a patient with diabetes. She was overweight, he thought, and thus responsible for the fact that she needed a foot amputation. But years later, Attia received an unpleasant medical surprise that led him to wonder: is our understanding of diabetes right? Could the precursors to diabetes cause obesity, and not the other way around? A look at how assumptions may be leading us to wage the wrong medical war.
Both a surgeon and a self-experimenter, Peter Attia hopes to ease the diabetes epidemic by challenging what we think we know and improving the scientific rigor in nutrition and obesity research.
Source: TEDMED - April 2013
Where Will You Choose to Swim Next Summer?
As the summer winds down, I could not help but be thankful for the fun we had in our backyard pool. It suddenly dawned on me that our private swimming pool provided many analogies as it relates to the direction of our federal health care reform initiatives. Many Americans, like my younger sister, will be the first to benefit from affordable coverage without any restrictions for preexisting conditions on January 1, 2014. The Affordable Care Act ("ACA") allows older Americans to pay a higher rate than younger Americans, but the community rating band will be broken down by only three different age groups. AARP lobbied strongly for this and it is an absolute boon to the baby boomers and a real shaft to Generation X, Y, and Millennials who will bear the brunt of the top third oldest risk tier by age. As an example, state exchanges will have age rating bands of 3:1 that will prevent insurers from charging an adult age 64 or older more than three times the premium they charge a 21 year old for the same coverage. Many believe the bands will be modified to reflect more of a 5:1 ratio as the individual market typically uses today.
Roughly 60% of Americans receive private health coverage through their employer. Think of each one of these employers as having their own swimming pool. When I look out at my own pool, our crystal blue waters are meticulously maintained by a cleaning crew that our family gets to select. When the job doesn't get done, we simply hire another supplier to get better results. We also get to decide who goes in and out of our family oasis (aside from a random duck that finds his way every year or so to the deep end). We have control over the environmental factors of our pool like if I want a salt-water or a chlorine pool. Additionally, we use brushers, skimmers and a Polaris as preventive measures that keep the water clean and healthy. This is not any different from an employer that sponsors their own corporate health and wellness plan.
On January 1, 2014, there will be another option - a public pool. When I was little I used to go to our community rec pool and my mom would pay to gain entry or buy a summer pass. Twenty-seven states (27) have agreed to run a community pool but do not really want to manage it. This leaves the cleanup and maintenance to a much larger pool cleaning company called the Federal Government. While Kathleen Sebelius and others will try hard to sell annual passes to younger Americans with lower health risk, there are three groups that will likely end up donning their swimming caps and jumping into the water:
a. Early retirees - This pre-Medicare eligible group is one of the most costly to have on your health plan with claims costs that are actuarially equivalent to three times that of the normal working population. A report by the Employee Health Benefit Research Institute (EBRI), shows around 17% of employers offered such coverage. The number of non-working early retirees who enroll through their employer is around 2 million lives. In a recent Aon Hewitt Survey, nearly a third of employers who provide early retiree coverage plan to direct them to the individual exchange market. Minnesota based 3M company is exhibit A here after eliminating their group plan for early retirees in favor of redirection to the public exchange pools in each state in 2014. This is typically done through transition credits through a health reimbursement arrangement (HRA). Not to blame 3M, as this is a rational market response when comparing premiums under three-tiered banded rates.
b. State continuation enrollees - As the insurer of last resort, state continuation enrollees and participants in the federal Pre-existing Condition Insurance Plan will be another group that will contribute to the losses in the state exchanges. About a quarter of a million Americans fall into this category with more than a dozen states declaring intentions to close their plans in the first six months of 2014. ACA provides a three-year transition period during which the costs of these programs will be shared across the market. However, many feel the $5 billion appropriation will not be enough to help states offset the costs through ACA.
c. Low-income Americans - There are numerous studies that unfortunately show a direct correlation between low-income wage earners who are uninsured and the propensity to be obese, have chronic illness and pre-existing conditions. This group will continue to be attracted to the community pool and have higher health risks when compared to their private plan cohort. While those who qualify for subsidies (household incomes of between 100-400% of the federal poverty level) are the ones who need it most, their risk factors should predictably drive costs higher each year over private plans. Over two-thirds of enrollment (CBO estimates) in the exchanges are anticipated to come from those receiving premium credits. This is something for employers contemplating "pay or play" moves should consider as a one year cost comparison may prove to be short-sighted without thinking through the tax implications and future trends of wading through the public waters.
What is the x-factor that will help keep public exchange costs in check? - those young invincibles ("Young-ens") with no claims who are predicted to enroll. Lets not count on them rushing in for fear of an underfunded IRS staff that will struggle to collect a paltry penalty (the higher of $95 per year or 1% of family income) from the uninsured. Keep in mind that ACA is a law whose details are unfamilair to two-thirds of Americans. Unless the IRS blocks access to the Young-ens X-Boxes until they join an Exchange, this group is going to take awhile to put on their swimming suits. Those of us who studied actuarial science and risk management in college know that the dreaded "death-spiral" can occur when younger healthier risks avoid the pool as costs go up leaving behind poorer risks with costs escalating higher each year.
Advice for Tending to Your Own "Swimming" Pool
An August 2013 Towers Watson survey confirmed that 98% of employers surveyed will retain their active medical plans for 2014 and 2015. The rationale given was that they view maintaining their own health plan (or swimming pool) as an important part of the employee value proposition and a competitive advantage for their companies.
My advice to my colleagues in senior level HR and Benefits who serve as the "lifeguards" of their private pools:
Hire the right crew and invest each year in preventive measures that deliver crystal clear waters.
Favorite Twit SteveSHarris
"Marry for love, not for health care" - Anonymous UPS Worker
— Steve Harris (@SteveSHarris) August 22, 2013
via http://twitter.com/SteveSHarris
39 Days Left - Employers Must Notify Employees of Health Insurance Exchanges
Section 1512 of the Affordable Care Act (ACA) requires companies in the U.S. with more than $500,000 in annual revenue to comply with a disclosure requirement no later than October 1, 2013. The requirement mandates that employers provide a notice to employees of coverage options available through their state exchange. All active employees, including both full and part timers, must receive the Marketplace Notice by October 1st, regardless of their enrollment in the employer plan sponsored group health plan. If an employee is hired after October 1st, the company has 14 days to get the notice to the employee.
If you have HR / Benefits responsibility, this an administrative task that should be outsourced to your communications advisor, benefits broker/consultant or COBRA / third-party administrator. Additionally, most carriers have already made arrangements to distribute notices on behalf of their clients who have fully-insured contracts.
White House Launches Website for Employers
Keeping up with the changes regarding health care reform is becoming a full-time job as key provisions have been delayed and legislatures are seeking ways to defund the law. To combat the information circulating on the web, The White House launched a new website for employers on health reform. The new site is located at BusinessUSA.gov/healthcare. The purpose of the site is to explain how key provisions of the Patient Protection and Affordable Care Act will work and impact health plan sponsors. This is one to bookmark to your favorites list whether you reside in a blue or red state.
Lighten Your Load or Pay More!
Lighten your load or pay more! This NPR report describes rationale for why it is permissible under the federal health reforms for employers to use incentive programs encouraged healthy behaviors.
Keeping It Real: From the Board Room to the Weight Room
This is the time of year when your employees are contemplating whether or not to eat that remaining peanut brittle or move on with 2012. For employers considering investing more in corporate wellness programs, we wanted to pass along a quick story and some rules for your folks who head to the gym. We recently visited with a prospective client who shared with us their meticulously overcooked wellness program where participants could receive points and olympic levels of achievement for enrolling online, taking tests, watching videos, and reaching out to coaches as "engaged" members. These "valuable" points could then be used to purchase a lot of left over things that retailers failed to sell over the holidays.
After listening intently how the employer was told the wellness plan would save the company a lost of money, we politely explained that this program was in reality money that could have been invested in a different way. Our Health Risk Solutions team will be doing more of these interventions throughout the year. For those who are not afraid of the truth ... our gift to you is Jason Gay's 27 Rules (as printed in today's WSJ) to share with your people:
1. A gym is not designed to make you feel instantly better about yourself. If a gym wanted to make you feel instantly better about yourself, it would be a bar.
2. Give yourself a goal. Maybe you want to lose 10 pounds. Maybe you want to quarterback the New York Jets into the playoffs. But be warned: Losing 10 pounds is hard.
3. Develop a gym routine. Try to go at least three times a week. Do a mix of strength training and cardiovascular conditioning. After the third week, stop carrying around that satchel of fresh-baked chocolate chip cookies.
4. No one in the history of gyms has ever lost a pound while reading "The New Yorker" and slowly pedaling a recumbent bicycle. No one.
5. Bring your iPod. Don't borrow the disgusting gym headphones, or use the sad plastic radio attachment on the treadmill, which always sounds like it's playing Kenny Loggins from a sewer.
6. Don't fall for gimmicks. The only tried-and-true method to lose 10 pounds in 48 hours is food poisoning.
7. Yes, every gym has an overenthusiastic spinning instructor who hasn't bought a record since "Walking on Sunshine."
8. There's also the Strange Guy Who is Always at the Gym. Just when you think he isn't here today...there he is, lurking by the barbells.
9. "Great job!" is trainer-speak for "It's not polite for me to laugh at you."
10. Beware a hip gym with a Wilco step class.
11. Gyms have two types of members: Members who wipe down the machines after using them, and the worst people in the universe.
12. Nope, that's not a "recovery energy bar with antioxidant dark chocolate." That's a chocolate bar.
13. Avoid Unsolicited Advice Guy, who, for the small fee of boring you to death, will explain the proper method for any exercise in 45 minutes or longer.
14. You can take 10 Minute Abs, 20 Minute Abs, and 30 Minute Abs. There is also Stop Eating Pizza and Eating Sheet Cake Abs–but that's super tough!
15. If you're motivated to buy an expensive home exercise machine, consider a "wooden coat rack." It costs $40, uses no electricity and does the exact same thing.
16. There's the yoga instructor everyone loves, and the yoga instructor everyone hates. Memorize who they are.
17. If you see an indoor rock climbing wall, you're either in a really cool gym or a romantic comedy starring Kate Hudson.
18. Be cautious about any class with the words "sunrise," "hell," or "Moby."
19. If a gym class is going to be effective, it's hard. If you're relaxed and enjoying yourself, you're at brunch.
20. If you need to bring your children, just let them loose in the silent meditation class. Nobody minds, and kids love candles.
21. Don't buy $150 sneakers, $100 yoga pants, and $4 water. Muscle shirts are for people with muscles, and rhythm guitarists.
22. Fancy gyms can be seductive, but once you get past the modern couches and fresh flowers and the water with lemon slices, you're basically paying for a boutique hotel with B.O.
23. Everyone sees you secretly racing the old people in the pool.
24. If you're at the point where you've bought biking shoes for the spinning class, you may as well go ahead and buy an actual bike. It's way more fun and it doesn't make you listen to C+C Music Factory.
25. Fact: Thinking about going to the gym burns between 0 and 0 calories.
26. A successful gym membership is like a marriage: If it's good, you show up committed and ready for hard work. If it's not good, you show up in sweatpants and watch a lot of bad TV.
27. There is no secret. Exercise and lay off the fries.
Source: Wall Street Journal, Jason Gay, The 27 Rules of Conquering the Gym